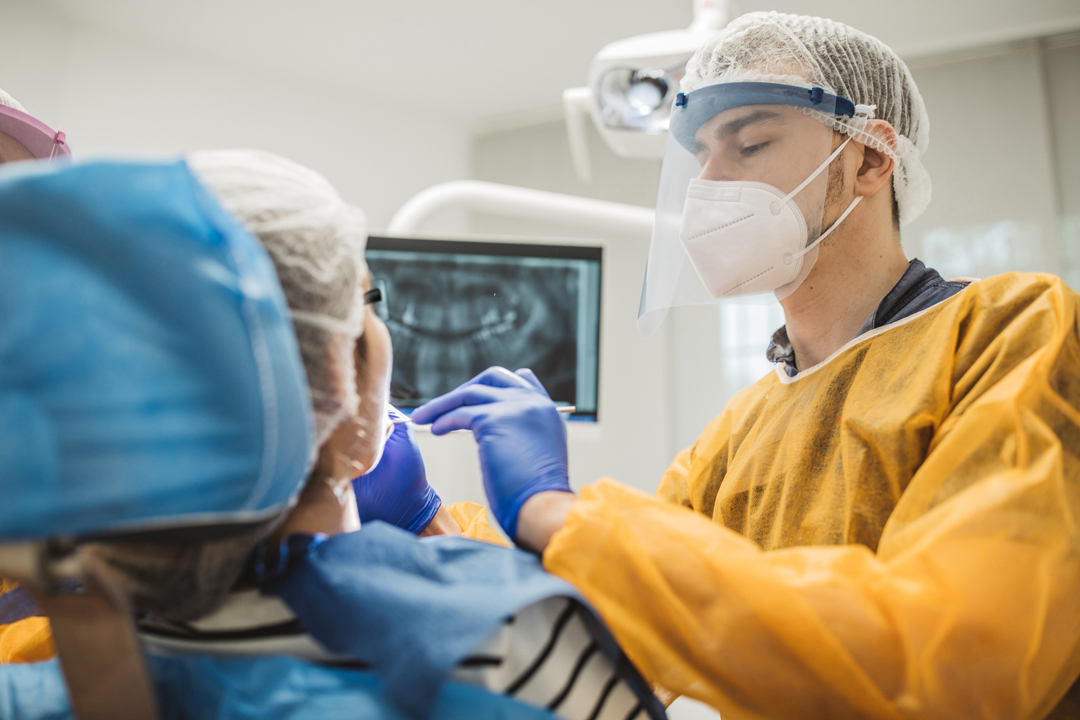
Dental group practices must have a clear understanding of the standard and its rationale to provide a sound respiratory protection program for all employees.
By Katherine Schrubbe, RDH, BS, M.Ed, PhD
The global pandemic of SARS-CoV-2 has had a huge impact on the dental profession regarding dental health care personnel (DHCP) safety and the safe delivery of dental care to patients. On March 16, 2020, the American Dental Association (ADA) recommended dentists nationwide postpone elective procedures for the next three weeks, stating that concentrating on emergency dental care will allow dentists to care for emergency patients and alleviate the burden that dental emergencies would place on hospital emergency departments.1 The closures went for much longer than three weeks and the recommendation that dentists restrict their practices to all but urgent and emergency care finally expired on April 30 and was not extended. At that point, the ADA stated, “oral health is an integral part of overall health and treatment of dental disease, as well as prevention, is important to help keep people healthy. The longer dental practices remain closed to preventive care and treatment for early forms of dental disease, the more likely that patients’ untreated disease will progress, increasing the complexity and cost for treatment down the road.”2
Dental practices were not only guided by ADA, but also had to follow state and local guidelines and mandates prior to reopening. However, in early to mid-May dental practices began to reopen to comprehensive procedures in states where government mandates began to lift. But it was not business as usual. Due to the many unknowns of the SARS-CoV-2 virus came new interim guidance from the Centers for Disease Control and Prevention (CDC) as well as the ADA on everything from patient screening, to operatory protocols and new recommendations for personal protective equipment (PPE). New interim guidance built upon the already strong infection control protocols in place in dental offices and called for the highest level of PPE to help protect patients and the dental team when re-engaging in providing the full range of oral health care.2
Since May 2020, there have been numerous revisions of interim guidance from the CDC, ADA and the Occupational Safety and Health Administration (OSHA) making compliance to new recommendations and protocols an ongoing daily activity – and challenge. The most significant change to dentistry practice during the SARs-CoV-2 pandemic is related to PPE and respiratory protection. Dental providers have always dealt with respiratory hazards in the workplace (i.e., spray, spatter and aerosols) and are the best at utilizing PPE under the premise that every patient is infectious. However, SARS-CoV-2 has generated a new level of concern given the high infectivity of the virus, the known risk of droplet transmission, as well as the potential for airborne transmission,3 thus, a higher level of PPE is recommended.
Current guidance
At the time of this writing, the most current CDC guidance for dentistry states, during aerosol generating procedures DHCP should use an N95 respirator or a respirator that offers an equivalent or higher level of protection such as other disposable filtering facepiece respirators, powered air-purifying respirators (PAPRs), or elastomeric respirators;
- Respirators should be used in the context of a comprehensive respiratory protection program (RPP), which includes medical evaluations, fit testing and training in accordance with OSHA’s Respiratory Protection standard (29 CFR 1910.134).4
In March, OSHA released Guidance on Preparing Workplaces for COVID-19 and outlined very high exposure risk jobs as those with high potential for exposure to known or suspected sources of COVID-19 during specific medical, postmortem, or laboratory procedures; workers in this category include healthcare workers (e.g., doctors, nurses, dentists, paramedics, emergency medical technicians) performing aerosol-generating procedures (e.g., intubation, cough induction procedures, bronchoscopies, some dental procedures and exams, or invasive specimen collection) on known or suspected COVID-19 patients.5 This guidance document highlighted the risk of transmission of SARS-CoV-2 to DHCP.
Although OSHA standards are federal law where employers must comply in order to maintain a safe workplace, during this unprecedented pandemic, in May, the agency created a webpage specifically for Dentistry Workers and Employers, stating, “this guidance is not a standard or regulation, and it creates no new legal obligations. It contains recommendations as well as descriptions of mandatory safety and health standards; the recommendations are advisory in nature, informational in content, and are intended to assist employers in providing a safe and healthful workplace.”6 With that, OSHA’s current respiratory protection PPE for dentistry during procedures that may or are known to generate aerosols include a NIOSH-certified, disposable N95 filtering facepiece respirator or better used as part of a comprehensive respiratory protection program that meets the requirements of OSHA’s Respiratory Protection Standard and includes medical exams, fit testing, and training.5,6 The ADA also refers to OSHA guidance for selection of respiratory PPE during the COVID-19 pandemic.6,7
The incorporation of OSHA’s Respiratory Protection Standard and the implementation of a Respiratory Protection Program (RPP) is a new area for dentistry and has created the need for more education, training as well as administrative tasks in the practice. If DHCP are donning respirators for aerosol generating procedures, then as OSHA has indicated, they must be used in the context of the standard and RPP.5,6,7
Reviewing the program
Without going into a great deal of discussion, let’s review the elements of a respiratory protection program for dental practice. According to OSHA, a respiratory protection program is a written program that includes procedures specific to the worksite to prevent inhalation of hazardous materials that cannot be controlled by other measures (i.e., engineering, or administrative controls).8,9 Along with the written RPP, OSHA requires the dental practice to designate the RPP administrator. This staff person may also be the safety officer for the practice and must be familiar with the Respiratory Protection Standard and the use and application of respirators in the workplace. Also, they are responsible to ensure DHCP are provided with an appropriate and suitable respirator that is provided at no cost by the employer to the employee, training, and medical evaluations to protect DHCP from inhaling harmful contaminants (contaminants could include biologic agents such as bacteria and viruses).8,9
The RPP includes the following elements:
- Procedure for selecting respirators for use in the workplace,
- Medical evaluation of employees required to wear respirators,
- Fit testing procedures for tight fitting respirators,
- Procedures for proper use of respirators in routine and reasonably foreseeable emergency situations,
- Procedures and schedules for cleaning, disinfecting, storing, inspecting, repairing, and discarding and otherwise maintaining respirators,
- Procedure to ensure adequate quality, quantity, and flow of breathing air for atmosphere-supplying air respirators,
- Training of employees in the proper use of respirators, including putting on and removing them, any limitations on their use and their maintenance,
- Procedures for regularly evaluating the effectiveness of the program, and
- Procedures for ensuring that workers who voluntarily wear respirators (excluding filtering facepieces) comply with the medical evaluation, and cleaning, storing, and maintenance requirements of the standard.8,9
There are a few key items that should be emphasized within the RPP. A written plan is required and should reside in the practice’s office compliance manual; with the program being reviewed regularly.8 DHCP have been sort-of thrown in to using respirators per CDC and OSHA guidance and practices are now finding there are additional tasks that need to be completed to comply with this standard. OSHA requires initial and annual fit-testing of respirators to ensure proper fit and seal, however, to preserve and prioritize the supply of respirators, OSHA has currently suspended its annual fit-test requirement, but continues to enforce an initial fit-test.10 Even before fit-testing is accomplished, DHCP must complete a medical evaluation to determine their eligibility of wearing a respirator.8,9 This medical evaluation consists of a lengthy health questionnaire evaluated by a physician or other licensed healthcare professional who provides a written recommendation regarding the ability to use respirators.9 For instance, if the DHCP has respiratory conditions such as asthma or severe allergies, they may not be able to obtain eligibility to wear a respirator. The practice should make every effort to comply with the fit-testing requirements to ensure DHCP safety. However, if it
is difficult to obtain a fit-test, the practice should document all attempts made to secure fit-testing services and continue to seek out this assistance.
As always, training is a vital component of any safety program, and the Respiratory Protection Standard mandates respirator training be provided prior to requiring an employee to use a respirator in the workplace. The training must be comprehensive, understandable, and recur at least annually – or more often if necessary.8,9
OSHA identifies the following as minimum knowledge a respirator user should have upon completing respirator training:
- Why the use of a respirator is necessary (e.g., the respiratory hazards and how improper fit, usage, or maintenance can compromise the protective effect of the respirator),
- Limitations and capabilities of the respirator,
- How to use the respirator effectively in emergency situations, including when
the respirator malfunctions, - How to inspect, don (put on) and doff (remove), use, and check the seals of the respirator,
- The procedures for maintenance and storage, and
- How to recognize medical signs and symptoms that may limit or prevent the effective use of the respirator.9
There has been a lot of conversation in dentistry regarding OSHA’s enforcement of the Respiratory Protection Standard since the start of the pandemic. Although OSHA is a complaint-driven agency, based on current information as of October 2, 2020, there appears to be plenty of complaints as OSHA has cited 37 establishments for violations, resulting in proposed penalties totaling $484,069 where employers failed to implement a written respiratory protection program, provide a medical evaluation, respirator fit test, training on the proper use of a respirator, and personal protective equipment.11 In September, OSHA cited a dental practice in Georgetown, Massachusetts for violating respiratory protection and other standards with proposed penalties of $9,500. The citation included failure to provide medical evaluations and fit testing for employees required to wear N95 respirators as protection against coronavirus and lack of written programs related to respiratory protection among other violations.12
Dentistry has been driven into a new “normal” of providing patient care that has added another layer of OSHA compliance to daily practice – the utilization of respirators for aerosol generating procedures requires the implementation of a respiratory protection program per the Respiratory Protection Standard. Employers and management teams must have a clear understanding of the standard and its rationale to provide a sound respiratory protection program for all employees. It should not be the potential for an OSHA citation that drives a dental practice to compliance, rather, it is the right thing to do to ensure DHCP safety.
References:
1. American Dental Association. ADA news. Available at https://www.ada.org/en/publications/ada-news/2020-archive/march/ada-recommending-dentists-postpone-elective-procedures. Accessed November 6, 2020.
2. American Dental Association. Available at https://www.ada.org/en/press-room/news-releases/2020-archives/may/as-dental-practices-resume-operations-ada-offers-continued-guidance. Accessed November 6, 2020.
3. Centers for Disease Control and Prevention. How covid-19 spreads. Available at https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/how-covid-spreads.html. Accessed November 6, 2020.
4. Centers for Disease Control and Prevention. Guidance for dental settings. Available at https://www.cdc.gov/coronavirus/2019-ncov/hcp/dental-settings.html. Accessed November 6, 2020.
5. US Department of Labor. Occupational Safety and Health Administration. Guidance on preparing workplaces for covid-19; March 2020. Available at https://www.osha.gov/Publications/OSHA3990.pdf. Accessed November 6, 2020.
6. US Department of Labor. Occupational Safety and Health Administration. Dentistry workers and employers. Available at https://www.osha.gov/SLTC/covid-19/dentistry.html. Accessed November 6, 2020.
7. American Dental Association. OSHA guidance summary: dentistry workers and employers; September 21, 2020. Available at https://success.ada.org/~/media/CPS/Files/COVID/OSHA_Guidance_Summary_Dentistry_Workers_And_Employers.pdf?utm_source=cpsorg&utm_medium=covid-resources-lp-safety&utm_content=cv-safety-osha-guidelines-dentistry&utm_campaign=covid-19. Accessed November 6, 2020.
8. US Department of Labor. Occupational Safety and Health Administration. Respiratory protection. Available at https://www.osha.gov/laws-regs/regulations/standardnumber/1910/1910.134. Accessed November 6, 2020.
9. Centers for Disease Control and Prevention. The national personal protective technology laboratory; respirator trusted source information. Available at https://www.cdc.gov/niosh/npptl/topics/respirators/disp_part/respsource3respirator.html#respb. Accessed November 6, 2020.
10. US Department of Labor. Occupational Safety and Health Administration. Temporary enforcement guidance – healthcare respiratory protection annual fit-testing for N95 filtering facepieces during the COVID-19 outbreak. Available at https://www.osha.gov/memos/2020-03-14/temporary-enforcement-guidance-healthcare-respiratory-protection-annual-fit. Accessed November 6, 2020.
11. US Department of Labor. Occupational Safety and Health Administration. OSHA national news release. Available at https://www.osha.gov/news/newsreleases/national/10022020-0. Accessed November 7, 2020.
12. US Department of Labor. Occupational Safety and Health Administration. OSHA national news release. Available at https://www.osha.gov/news/newsreleases/national/09162020. Accessed November 7, 2020.